Until this weekend, it had never crossed my mind that having a dental extraction could lead to a nasty complicated fracture of the ankle.
We were working nights this weekend – at 7pm we’d checked the vehicle over, replaced a couple of items and were ready for our first call. When it came, I went out to the vehicle and looked at the screen.
“Dental extraction this afternoon, passed out, injured broken ankle”
I got the dental extraction bit (I’ve got to have a couple extracted myself – NOT looking forward to it as I have a very real fear of dentists), I got the passed out bit, but I didn’t get the broken ankle bit. Did it mean the broken ankle was an old injury, or did it mean that the act of passing out had caused the broken ankle? I pondered the possibilities as my crewmate Graham drove us to the call.
We were met by the patient’s brother. “He’s in the living room, he passed out upstairs and he’s got a very nasty injury to his ankle.”
“Ok.”
Our patient, Al, was sitting on a chair with his right leg crossed over his left. His right foot dangled uselessly in mid-air, a large lump on his ankle was being held in place by his sock through which blood seeped and dripped steadily onto a towel on the floor underneath.
I turned to Graham.
“Vacuum splint, Entonox, and carry chair please.” Graham left to fetch the necessary equipment.
Al explained he’d had a tooth extracted at lunchtime, and since then, he’d been getting large blood clots forming in his gum which when they came away, he was spitting down the toilet upstairs. On the last trip to expel another clot, he’d passed out in his bathroom, and when he woke up, he was on the floor and his right foot lay at ninety degrees to his leg. He was on his own at this point, but knew he had to get help, so he’d somehow managed to come downstairs on his bottom, and phoned his brother who lived just down the road and had a key to get in. His brother had taken one look at the ankle and called us.
I was amazed at how calmly Al was just sitting there with his clearly badly injured ankle, chatting away as though there was nothing wrong. “Al, out of ten, zero being no pain, and ten being the worst pain you’ve ever experienced, how painful is your ankle?”
“Oh, about three out of ten.” I’d have been screaming.
Graham returned, and after starting Al on Entonox (gas and air), we set about removing the shoe and sock from his right ankle. With a bit of care, we were able to remove his shoe without the need to cut it off, but we had to cut his sock. As we peeled the sock away from his ankle, we saw the bottom of the Tibia (shin bone), known as the Medial Malleolus, poking through the skin on the inside of his ankle. He had not only fractured his ankle, but had dislocated it as well.
A steady stream of blood came from the wound. I felt Al’s foot for temperature and for a pulse, checking that the fracture dislocation hadn’t disrupted the blood supply to the foot. The foot was warm, and I found the pulse on the top of his foot. The pulse can be quite difficult to find, so when we do find it, we put a pen mark at the right point. We then gently put a pad and bandage over the wound, and placed his leg in a vacuum splint. As the name suggests, we wrap the splint around the leg, then using the suction unit, we suck the air out, and the splint moulds itself to the injury and sets hard, preventing movement.
Having his leg straight increased the pain in his ankle, so we gave him some morphine, and took him out to the ambulance.
Due to the nature of the injury, we decided to let the hospital know so they could get an orthopaedic specialist down and we took him in on blue lights.
Later when we went back with another patient, Al had had his leg put in plaster. He told us that he was to have an operation the next day to have his ankle pinned back together. The orthopaedic specialist showed me the x-ray.
This is a normal x-ray of a right ankle. The view is from the front, as though the person was standing facing you.
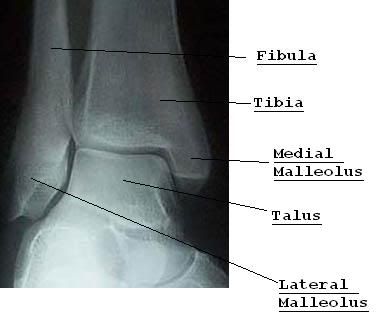
Al’s x-ray showed the Medial Malleolus had moved sideways – to the right as you look at the x-ray. It also showed that he had a Spiral fracture at the lower end of the shaft of his Fibula – if you were to imagine a spiral staircase going up the outside of the shaft of the bone, that’s what it looked like on the x-ray, but without the steps.
In the operation, the Medial Malleolus would be put back in the correct place, and pinned in place to the Talus. Pins would also be placed along the broken shaft of the Fibula to hold it in place to ensure it repaired correctly.
It was nice to get this feedback from the Dr. All too often we take people to hospital and don't get to know the outcome. It's as frustrating for us as it is for you reading ambulance blogs, because we use this feedback to confirm our own provisional diagnosis, and where that doesn't match, as learning points, to help us to recognise injuries and illnesses and give better treatment in future.



